Constipation/Encopresis
Constipation
Constipation is a common problem in children causing 5% of the visits to the pediatrician and 30% of visits to the gastroenterologist.
In children older than 1 yr of age 95% of the cases its cause is functional, and only 5% of them have an organic cause
.It is important to address this issue when young because 25% of children with constipation will continue to have issues into adulthood.
How does it all work?
The transit of the colon works in response to intestinal contractions. In infants these can happen 6-7 times a day and happen even at rest. As kids get older they decrease in frequency. The most common one happens in response to a meal and distention of the stomach... "the gastrocolic reflex".
As the rectum, the last part of the colon, fills up with stool and gets distended, the sensation or urge to have a BM is created.
The colon is an elastic organ, and like a "scrunchy" as it gets stretched or distended, it looses it's elasticity and the fibers can't contract as effectively. This causes loose of sensation or "urge" and weaker muscles.
The rectum job is to reabsorb water from the stool while it is there, and it continues to do so even when the stool has been there for a few days, making the stool harder and larger.
The combination of larger and harder stools, with weaker rectum muscles and lower sensation, and with the same size anus causes pain when having a BM, trauma and holding behavior.
Stool accidents can be of 2 types:
- younger child who is spending most of the time holding the stool, the moment they relax a small amount of formed stool comes out.
- older kids who are impacted with large stool and do not completely empty the rectum, liquid stool can seep through without them being aware that it is happening.
Treatment and rehabilitation can restore normal colonic function but in order to be successful every part of the cycle has to be addressed.
What is considered constipation?
- Hard or painful stools
- 2 or less stools a week
- Blood with wiping
- Soiling in the underwear, which could be of loose consistency or small formed stools (encopresis)
- Have large BMs that stop up the toilet.
- Holding: clench their bottom when having the urge. Although this behavior may look like your child is trying to push the stool out, they may be really trying to hold it in because it hurts to come out.
What causes constipation?
- Holding could be caused by:
- pain when passing a hard and/or large stool.
- power struggles: between 2 to 5 years, children may want to show they can decide things for themselves. Holding back their stools may be their way of taking control. It is best not to push children into toilet training.
- don't want to stop their activity in order to go to the bathroom.
- Diet. Not enough fiber or liquid in your child's diet does't cause constipation. However,
not consuming enough of the recommended amounts of healthy foods from the 5 food
groups, including foods that are good sources of fiber, may affect your child's bowel
patterns. (See the How much fiber does my child need? section.)
- Other changes. In general, any changes in your child's routine, such as traveling, hot
weather, or stressful situations, may affect his overall health and how his bowels
function. Older children may hold back their stools when away from home (such as camp
or school). They may be afraid of or not like using public toilets.
Treatment
GOAL: soft stools 5-6 times a week.
Chronic constipation causes the colon to be unresponsive to stool accumulation due to distension and effective treatment requires consistent and complete emptying of the colon, so that it becomes conditioned to work on its own. This concept is known as "bowel retraining".
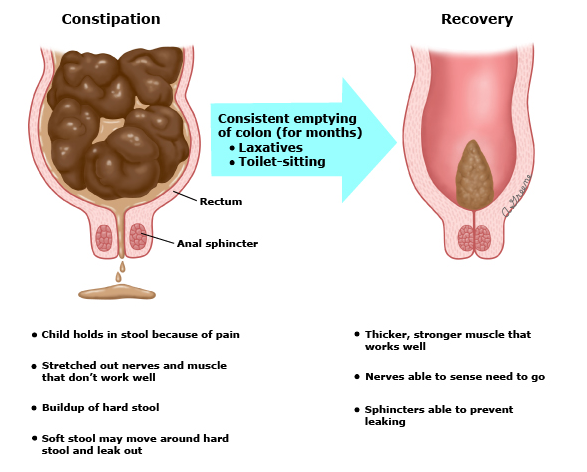
There are four general steps in bowel retraining and your provider will tell you where your child should start.
- Disimpaction (for children with a large rectal stool mass or fecal incontinence
- Prolonged daily maintenance treatment with stool softeners and behavioral therapy to achieve regular evacuation and avoid recurrent constipation
- Dietary changes (primarily increasing fiber and fluid content) to maintain soft stools
- Gradual tapering and withdrawal of laxatives as tolerated
Disimpaction
This can be achieves with oral medication, rectal medication or a combination of both.
Day 1
Oral: For most children, we suggest an oral regimen for disimpaction because this method is noninvasive and may help the child feel in control. Oral medications also are particularly valuable for children with a history of painful stools or difficulty tolerating enemas. Sometimes it is hard to keep up with the amount of liquid necessary to be taken to reach the goal of very soft, difficult to hold stools.
1. In children older than 2 yrs of age take stimulant medication 30 minutes before starting to drink the Miralax mixture
- 2-3 yrs old: 1/2 chocolate square of Exlax (senna)
- 3-12 yrs old: 1 chocolate square of Exlax chewable or Dulcolax (1 tab a day, 5 mg)
- > 12 yrs old: 2 chocolate square, or Dulcolax (bisacodile laxatives) ,2-3 tablets once a day, 10-15 mg
2. Mix Miralax/polyethylene glycol(PEG) with non carbonated liquid like water, juice or Gatorade. Do not mix with milk or pop) and drink 1/2 of the total amount in the morning, and drink the other half in the afternoon. Can keep in the refrigerator to help with the flavor.
3. 1-2 hrs after finishing Miralax should start passing stool that will become thinner and clear.
It is helpful to have a clear liquid diet during the day this is done to maximize it's response.
Laxatives like exlax or dulcolax will cause "abdominal pain", and that is when the child should go to the bathroom to pass stool. Explain this will resolve once clean out is completed. Warm baths can sometimes help with the cramping.



Rectal: For patients with severe impaction, rectal medications may be needed and are typically used in combination with oral medications. Rectal medications are more rapidly effective than oral medications for disimpaction and may be a powerful motivator for sitting on the toilet. However, we avoid their use except in patients with severe impaction because enemas are invasive and may be difficult to administer to an uncooperative or fearful child.
- less than 2 yrs old can use glycerin suppositories
- 2-5 yrs old liquid glycerin suppositories like Pedia-lax
- 2-12 yrs old 1/2 of the 4.5 oz bottle of a mineral oil enema like fleet enema. (read ingredients of enema carefully)
- >12 yrs old 4.5 oz bottle of mineral oil enema
We do not recommend sodium phosphate enemas, or ones made of soapsuds, tap water, milk and molasses, magnesium or herbal formulations.
After enema is done start with PEG/Miralax daily in combination with a stimulant laxative daily.
It is helpful to have clear liquid diet during the day of the clean out as well.


Day 2
Repeat Step 1 and 2 from day prior.
Laxatives like ex-lax or Dulcolax can cause “abdominal pain” and that is when child should go to the bathroom.
Laxatives like Exlax or dulcolax will cause "abdominal pain", and that is when the child should go to the bathroom to pass stool. Explain this will resolve once clean out is completed. Warm baths can sometimes help with cramping.
Maintenance treatment with stool softeners and behavioral therapy
Day 3
Soft stools are the key to helping children overcome the fear of using the toilet given that they have weak muscles and they are afraid of having painful stools.
1. give 1/2 to 1 cap of Miralax in 8 oz of fluid. Increase or decrease the amount for goal of chocolate pudding like stools and continue this for the next 2 months.
2. some children may need the Exlax/dulcolax during the first week if after a few days you see that no stools are passing. Give it in the afternoon for the next week with goal of having a stool by the end of the day.
Stimulant laxative options:
If your child is a stool holder, they may benefit for continue to take stimulant laxatives (i.e. ex-ex lax, dulcolax).
Give the laxative with goal of it taking effect at toilet scheduled time. (see below). This will help those who have lost the sensation/urgency, and those who are stool holders.
Do not use for more than 2 weeks.
Stool softeners options:
-Miralax daily (preferred choice) with non carbonated drink or water, to be taken in 30 minutes or less for it to work. It is best to give it after school and/or before dinner. Do not give at bedtime.
- Magnesium: milk of magnesia or magnesium oxide gummies, daily.
Continue the daily dose of the chosen stool softener to achieve the goal of soft stools 6-7 stools a week.
Re-training in chronic constipation cases can take a minimum of 3 months.
When/if stool holding continues, or the dietary changes have not been successful your child may have to continue with the daily stool softener of choice to prevent regression to the stool holding and constipation pattern.
Behavioral therapy (only for those who are toilet trained)
This will include toilet sitting and a reward system.
Toilet sitting
- sit in the toilet shortly after a meal for 5-10 min 1-2 times a day
- same time every day and use a timer
- The routine should be followed every day, particularly during times of transition (eg, holidays, vacations, or weekends)
- The child's adherence to the program should be encouraged with positive reinforces, as described below, rather than negative reinforces (criticism or punishment)
- For children whose feet do not touch the floor sitting on a regular toilet seat, it is helpful to use a stool for foot support. A foot support that raises the knees above the level of the hips can help relax the pelvic floor and is particularly helpful for a child who tends to withhold stool.
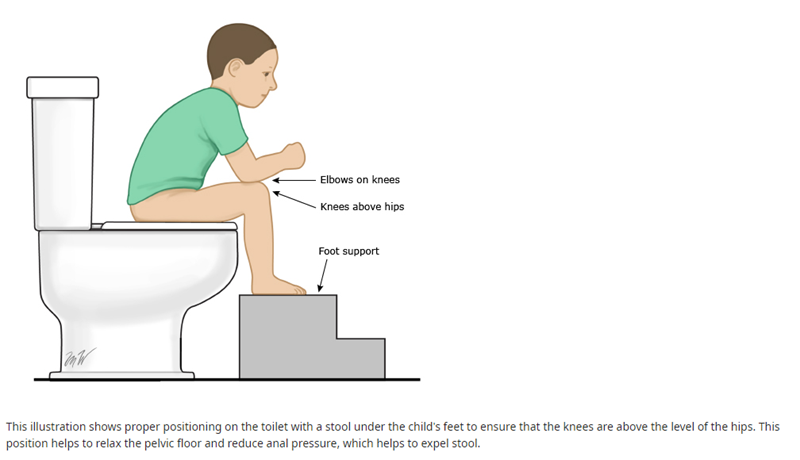
Reward system
- the reward is provided for effort (i.e, toilet sitting) rather than success (i.e, evacuation in the toilet)
- give a reminder 15-30 min after dinner, "Its time to sit", 1 min per year of age, max of 10 min.No screen, actively trying to have a stool.
- examples of rewards for preschoolers may include stickers or small sweets, reading books or special toys that are only used after toilet sitting
- examples of rewards for school-aged children may include reading books together, activity books, or hand held computer games that are only used after sitting time or coins that can be redeemed for small drug store items.
We recommend using a stool chart for tracking and marking efforts than can be brought to you next follow up visit.
See example below
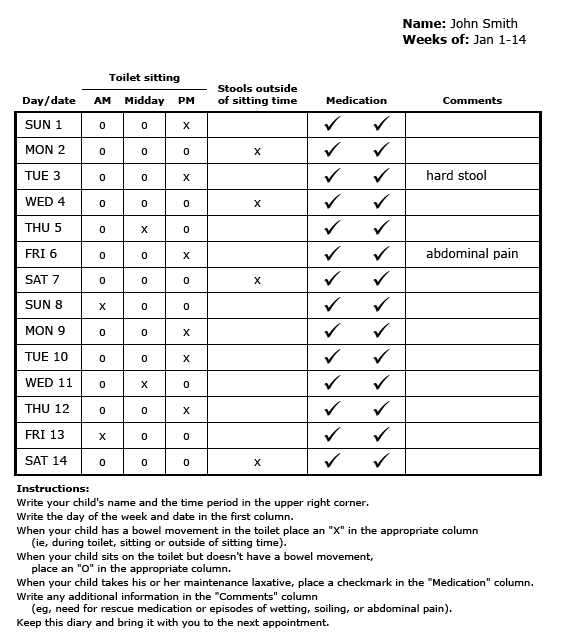
Stool Link PDF Below
Relapses are common, and if after achieving regularity had 3 days with no stool, may have to increase PEG/Miralax dose, or may need one or 2 doses of a stimulant laxative like senna or bisacodyl.
If successful go back to regular schedule but increase the daily dose PEG/Miralax adjusting for a goal of a soft stool.
Dietary changes
Fluid intake – To ensure adequate hydration, children with chronic constipation or fecal incontinence should be encouraged to consume at least 32 to 64 ounces (960 to 1920 mL) of water or other nonmilk liquids per day, particularly if they are using fiber supplements. Contrary to popular belief, there is no evidence that constipation can be successfully treated by increasing fluid intake unless the patient is clinically dehydrated.
Fiber - To prevent constipation, a practical target for fiber intake is the child's age plus 5 to 10 grams per day. Giving more than this fiber goal has no proven benefit for the management of constipation in children.
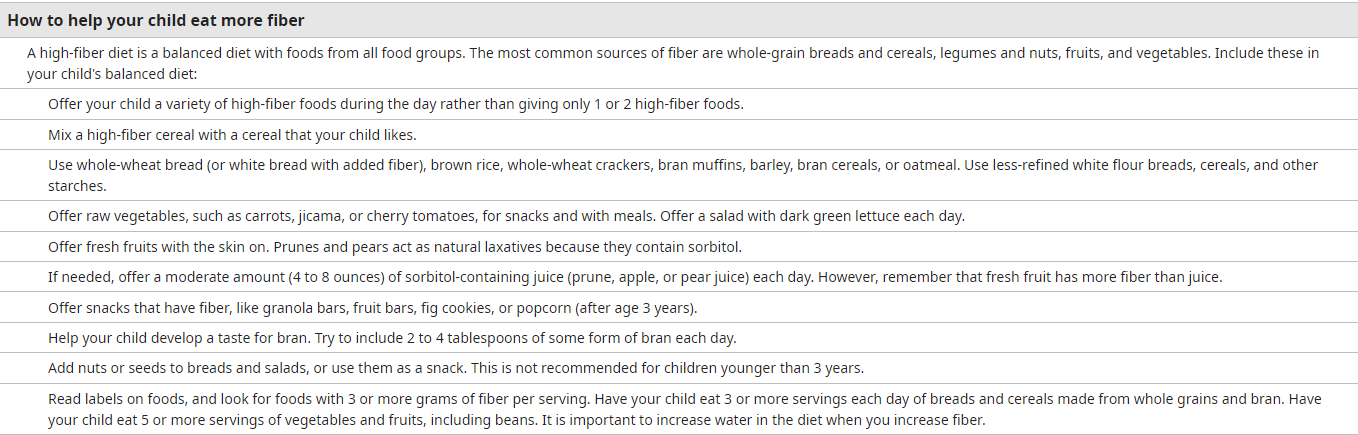
Fiber content of common foods
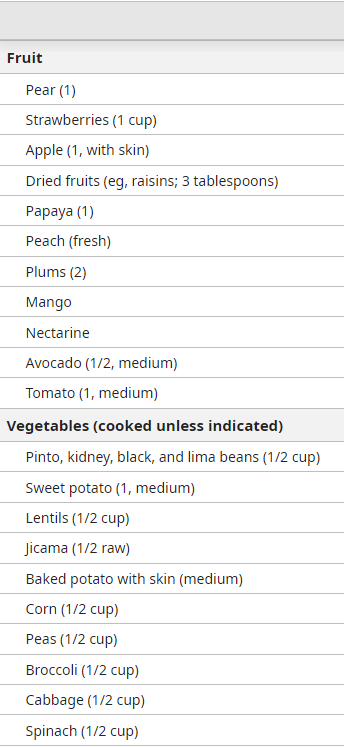
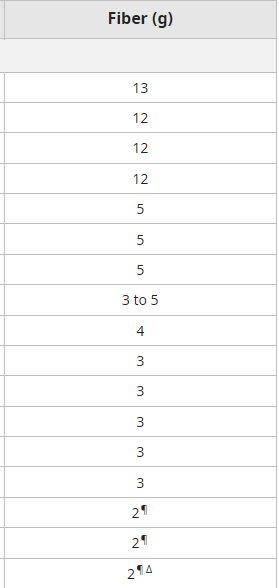
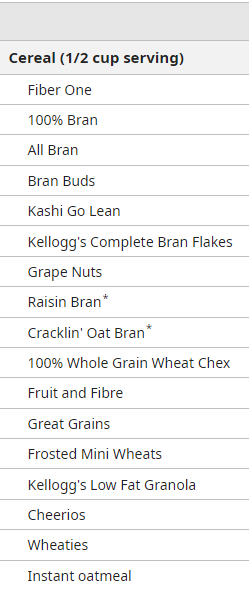
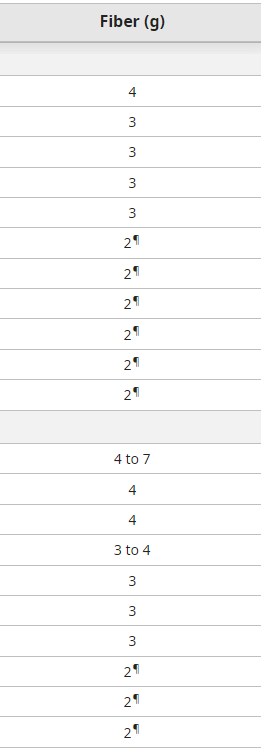

Tapering laxative therapy
Once the child has achieved regular bowel habits (and independently uses the toilet), the frequency of mandatory toilet sitting and the use of laxatives can be reduced. The laxative dose is gradually decreased to a dose that will prevent fecal incontinence and maintain one to two bowel movements per day.
We typically wait until optimal bowel habits are achieved and stable for at least six months before laxative use is further decreased or discontinued. In many cases, laxatives need to be taken for months and sometimes years to maintain daily soft stools. Stopping laxatives too soon will likely lead to a prompt recurrence.
As laxative therapy is discontinued, it is particularly important to continue a healthy high fiber and balanced diet.
The parents and child should have a "rescue" plan which may involve the use of an enema or suppository, followed by an increase in the laxative dose. The development of such a plan empowers the child and family to anticipate, tolerate, and treat recurrences.
See video below which helps summarize the main issues to address.
For more information and questions you can contact our office and schedule a visit with one of our providers.



