ADHD
Attention Deficit Hyperactivity Disorder (ADHD) is a developmental disorder that affects the behavior, attention, and learning of children. Diagnostic criteria for ADHD include symptoms of hyperactivity, impulsivity, and/or inattention that occur in more than one setting (school and home), affect function (eg, academic, social, emotional, etc).
It is a chronic disorder with therapy ranging from behavioral modifications to treatment with medication. Treatment of ADHD may involve behavioral interventions, medication, school-based interventions, or psychologic interventions alone or in combination.
Understanding The Scattered (ADHD) Brain
Clinical Symptoms
ADHD is a syndrome with two categories of core symptoms: Hyperactivity/Impulsivity and Inattention. The complaint regarding symptoms of ADHD may originate from the parents, teachers, or other caregivers.
Hyperactivity and Impulsivity
Hyperactive and impulsive behaviors almost always occur together in young children. The predominantly hyperactive-impulsive subtype of ADHD is characterized by the inability to sit still or inhibit behavior. They may include:
- Excessive fidgetiness (eg, tapping the hands or feet, squirming in seat)
- Difficulty remaining seated when sitting is required (eg, at school, work, etc)
- Feelings of restlessness (in adolescents) or inappropriate running around or climbing in younger children
- Difficulty playing quietly
- Difficult to keep up with, seeming to always be "on the go"
- Excessive talking
- Difficulty waiting turns
- Blurting out answers too quickly
- Interruption or intrusion of others
Inattention
Children with the inattentive subtype often are described as having a sluggish learning tempo and frequently appear to be daydreaming or "off task". The typical presenting complaints center difficulty learning and doing poorly in school. Symptoms of inattention may include:
- Failure to provide close attention to detail, careless mistakes
- Difficulty maintaining attention in play, school, or home activities
- Seems not to listen, even when directly addressed
- Fails to follow through (eg, homework, chores, etc)
- Difficulty organizing tasks, activities, and belongings
- Avoids tasks that require consistent mental effort
- Loses objects needed for homework or activities (eg, school books, sports equipment, etc)
- Easily distracted
- Forgetfulness in routine activities (eg, homework, chores, etc)
The symptoms of inattention typically are not apparent until the child is eight to nine years of age. This delay may relate to reduced sensitivity of assessment of attention problems or increased variability in the normal development of the cognitive skills.
Evaluation
Evaluation for ADHD
Should be initiated in children older than 4 years of age who have symptoms of inattention, hyperactivity, or impulsivity or who have complaints frequently associated with ADHD (eg, poor school performance, difficulty making and keeping friends, difficulty with team sports).
The evaluation for possible ADHD includes comprehensive medical, developmental, educational, and psychosocial evaluation.
Comprehensive evaluation is necessary to determine the presence, persistence, and complications determined by the diagnosis of ADHD, and identify other coexisting emotional or behavioral diagnosis.
Re-Evaluation of children with ADHD is warranted whenever symptoms worsen or new symptoms emerge because the differential diagnosis of ADHD is extensive and comorbidity is common.
Diagnosis
Diagnosis for ADHD
- For children <17 years, diagnosis of ADHD requires ≥6 symptoms of hyperactivity and impulsivity or ≥6 symptoms of inattention.
- For adolescents ≥17 years and adults, ≥5 symptoms of hyperactivity and impulsivity or ≥5 symptoms of inattention are required.
The symptoms of hyperactivity/impulsivity or inattention must:
- Occur often
- Be present in more than one setting (eg, school and home)
- Persist for at least six months
- Be present before the age of 12 years
- Impair function in academic, social, or occupational activities
- Be excessive for the developmental level of the child
Kidz1st can provide you with information regarding where this evaluation can take place.
Treatment Types
Medications
(see detailed information at the bottom of the page)
- Medications, with or without behavioral/psychologic interventions, are the first-line therapy for children 6 yrs and older, and adolescents with ADHD.
- Medications may be used together with behavioral interventions for preschool children (4 through 5 years) who fail to respond to behavioral interventions alone.
Behavioral Interventions
Behavioral techniques that are used for children with ADHD include positive reinforcement, time-out, response cost (withdrawing rewards or privileges when unwanted or problem behavior occurs), and token economy (a combination of positive reinforcement and response cost).
Behavior therapy and environmental changes that can be used by parents or teachers to shape the behavior of children with ADHD include:
- Maintaining a daily schedule
- Keeping distractions to a minimum
- Providing specific and logical places for the child to keep his or her schoolwork, toys, and clothes
- Setting small, reachable goals
- Rewarding positive behavior (eg, with a "token economy")
- Identifying unintentional reinforcement of negative behaviors
- Using charts and checklists to help the child stay "on task"
- Limiting choices
- Finding activities in which the child can be successful (eg, hobbies, sports)
- Using calm discipline (eg, time out, distraction, removing the child from the situation)
Additional tips for parents of children age 6 to 12 years are available through the National Initiative for Children's Healthcare Quality toolkit, free with registration.
Standardized training programs for parents of preschool children with disruptive behavior disorders (including symptoms of ADHD) include:
- Incredible Years Parenting Program
- New Forest Parenting Program (specifically designed to address ADHD symptoms)
- Positive Parenting Program (Triple P)
- Parent-Child Interaction Therapy
- Helping the Noncompliant Child
A great resource to help look for counselors can be found at Psychology Today.
Combination Therapy
Combination therapy uses both behavioral/psychologic interventions and medications. Studies have shown that combination therapy with medications and behavior/psychologic therapy was superior to behavior/psychological therapy alone.
Unproven Treatments
- Elimination Diets: We generally do not suggest elimination diets for children with ADHD, but decisions regarding trials of dietary interventions for ADHD must be made on a case-by-case basis. The influence of diet on attention, hyperactivity, and behavior is controversial. Dietary factors (eg, food additives, food allergy or intolerance, etc) generally do not impact behavior to a clinically significant level and do not account for the majority of cases of ADHD. However, a small subset of children may demonstrate mild adverse behavioral effects in response to particular dietary components and improvements in behavior when these components are eliminated.
- Others: Fatty acid supplements, trigeminal nerve stimulation, vision training, megavitamins, herbal and mineral supplements (eg, St. John's wort), neurofeedback/biofeedback, chelation, and applied kinesiology, among others.
IF ANY OF THESE ARE USED, PLEASE LET US KNOW.
Genetic Testing
We do not recommend performing pharmacogenetic testing before prescribing medication for ADHD.
We agree with the US Food and Drug Administration and the American Academy of Pediatrics that results of pharmacogenetic tests that are directly marketed to consumers should not be used to make decisions about the appropriateness of a particular medication or dosing of such.
Treatment Goals
It is important to have realistic, achievable and measurable target goals when treating ADHD. These may change with time and should be created between the parent, patient and school. Some examples of goals are:
- Improved relationships with parents, teachers, siblings, or peers (eg, plays without fighting at recess)
- Improved academic performance (eg, completes academic assignments)
- Improved rule following (eg, does not talk back to the teacher)
Treatment of Co-Existing Conditions
As many as one-third of children with ADHD have one or more coexisting conditions (eg, learning disabilities, oppositional defiant disorder, conduct disorder, anxiety disorder, mood disorders, tics, sleep disorders). It is important that those are addressed as well since it may influence the success of treatment of the ADHD
Behavioral and psychologic interventions may be necessary for managing the full spectrum of symptoms. Treatment of sleep problems may improve ADHD symptoms as well.
School-Based Interventions
School-based interventions may include tutoring or resource room support, classroom modifications, accommodations, or behavioral interventions.
Classroom modifications and accommodations may include:
- Having assignments written on the board
- Sitting near the teacher
- Having extended time to complete tasks
- Being allowed to take tests in a less distracting environment
- Receiving a private signal from the teacher when the child is "off-task."
The teacher's completion of a daily report card facilitates the monitoring of symptoms and the need for changes in the treatment plan.
In the United States, ADHD is considered to be a disability under the Individuals with Disabilities Education Act (IDEA [PL-101-476]). Under IDEA, children with ADHD may qualify for special education or related services. Alternatively, they may qualify for appropriate accommodations within the regular classroom setting under Section 504 of the Rehabilitation Act of 1973.
In addition, the Americans with Disabilities Act may provide individuals with ADHD reasonable accommodations in secular private schools and post-secondary education The completion of a daily report card or a "communication book" to facilitate communication between the parents and the teachers may be suggested as an accommodation under a 504 plan.
Once a diagnosis is made, regular monitoring of the effectiveness of treatment is important. Frequent communication between the teacher, parents and health care provider is necessary to ensure optimal treatment and success for the child.
THE EVALUATION IS DONE..... NOW WHAT???
Once your child has completed the evaluation and the diagnosis of ADHD has been made, you are ready for your child to have his initial ADHD visit with Dr. Operti-Considine.
Because of the intricate treatment of ADHD, it is important that your child is up to date with his annual exam. This will be extremely helpful in making the best treatment recommendation by having updated and complete information on your child.
A copy of the evaluation is needed so it can be reviewed prior to the appointment visit.
Please know that ADHD treatment and management is a group effort which involves the parent, the teachers, the child/adolescent and the doctor. Open communication and understanding is a MUST for us to be able to help your child be the best they can be. We will STRONGLY encourage you to sign your child in our office portal. This will allow for direct an open communication between parents and our office which can be used for refill requests, questions, updates and much more. (Reminder - NOT TO BE USED IN CASE OF AN EMERGENCY)
Once medication management is established and well controlled, office visits every 3-6 months will be done. At these visits, valid follow up questionnaires completed by your child’s teacher and parent will be reviewed to help identify response to therapy, any side effects of medication as well as any other concerns. When medication is being changed, more frequent follow ups may be necessary.
Since the medication used for ADHD is a controlled substance, a maximum of 30 days of treatment may be requested at a time. The prescriptions can be e-prescribed and should be requested through our portal. It is recommended that 4-5 days prior to needing a new prescription, a message with the request is sent through the portal. If not able to, please contact our office for further instructions. Once the refill has been sent to the pharmacy you will receive a response through our portal confirming the script has been sent. If such message is not received please contact our office for follow up.
If your child is not up to date with the well exams and requested medication rechecks, refills of the medications will not be provided.
Helpful Websites
We strive to treat and manage our patients with evidence-based research recommendations. The internet provides a vast amount of anecdotal and non-research based material regarding ADHD.
The websites below offer evidence based information regarding ADHD. Please refer to them for more information.
- Healthy Children (AAP Parenting Website) - Articles on ADHD
- CHADD (Children and Adults with ADHD) - National Research Center on ADHD
Book Recommendation
- ADHD - What Every Parent Needs to Know by Michael L. Reiff
More Information On Medications
Stimulant vs Other Medications
When we agree to a trial of medication for ADHD in a school-aged child or adolescent (≥6 years), we suggest a stimulant as the first-line medicine.
Stimulants are preferred to other medications because they have a rapid onset of action and long record of safety and efficacy.
Non-Stimulant Medications
Selective norepinephrine reuptake inhibitors (Strattera, Qelbree) are alternatives. Strattera is less effective than stimulants but well tolerated.
Alpha-2-adrenergic agonists (guafenicin/Intuniv, or clonidine) usually are used when children respond poorly to medications above. By themselves they are less effective than stimulants.
They are sometimes used together with a stimulant to maximize the effect of the stimulant when a higher dose is not tolerated, or can be used to help patients with sleep or other behavioral issues.
At least 80 percent of school-aged children and adolescents will respond to one of the stimulants.
In addition to improvement with the main symptoms of ADHD, treatment with stimulants can also improves family interactions, aggressive behavior, and academic productivity and accuracy.
Stimulant Medications
Stimulant medications do not significantly affect learning problems, reduced social skills, oppositional behavior, or emotional problems that are secondary to or coexist with ADHD.
However, stimulant medications may facilitate the treatment of these problems by controlling the core symptoms of ADHD. In addition, the use of stimulant medications may improve self-esteem.
General Considerations for Choosing Medication
The choice of the initial medication depends upon a number of factors, including:
- How long we want the medication to work for (completion of homework or driving may require coverage into the evening)
- If the patient can swallow pills (helps to have practice with tic-tacs)
- Expense: we will be working with you and your insurance to make sure that treatments are affordable. Information on websites for price comparison and coupons will be shared when available.
Generic drugs are less expensive than brand-names but not available for all formulations. Some have more than one manufacterer. If generics are used and your child responds well to them, we encouraged that you become familiar with the name and look of the capsule or tablet.
Pharmacies and insurances sometimes make changes unbeknowns to us and you which could be associated to a difference response in your child.
Comparison Table Showing Different Stimulant Medications
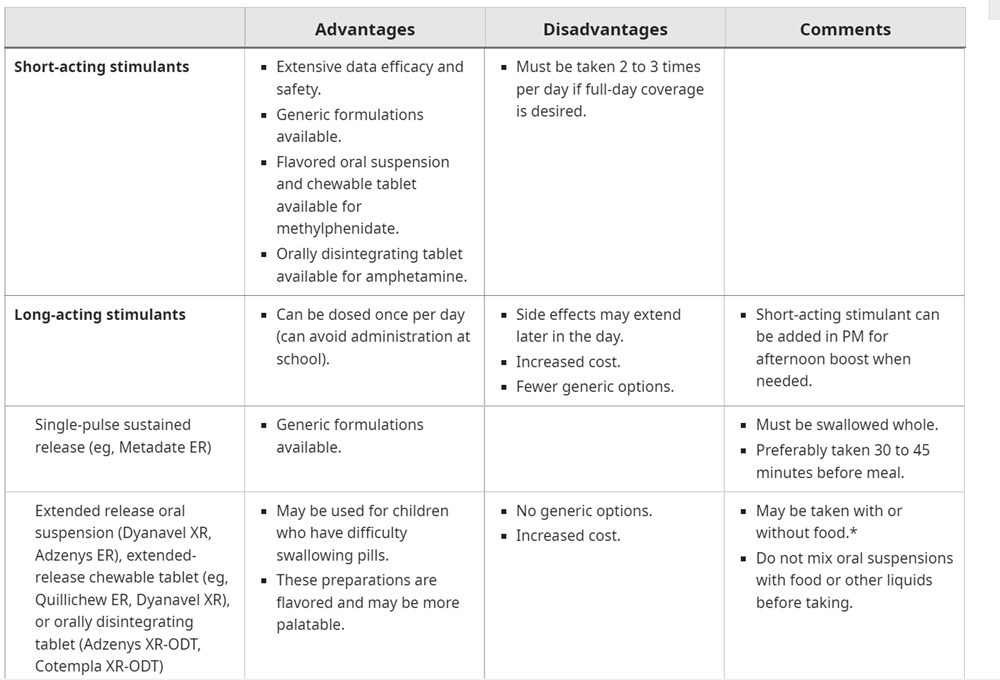
Managing Stimulant Side Effects
When children or adolescents who are being treated with stimulant medications develop adverse effects, It is important to gather as much information as possible in order to help us determine if these are related to the medication or time it is given,; or is related to other factors, i.e. stressors, or other pre-existing issues.
Mild adverse effects may resolve with time or can be addressed by adjusting the dose, time of administration, or formulation of stimulant.
Tips for initial management of common adverse effects of stimulant medications are provided below:
- Decreased appetite – Administer the medication at or after a meal; encourage the child to eat nutrient dense foods before those with "empty calories;" offer food that the child likes for the noon meal, which is the meal most commonly affected. It is also important to become aware of when the medication is wearing off, and therefore the child is more hungry. This will help us adjust meal time, or have a "second dinner" ready for when that happens.
- Insomnia/nightmares – Establish a bedtime routine and good sleep habits; or administer earlier in the day.
- Rebound – "Rebound" refers to symptoms or adverse effects that occur as the medication is wearing off; rebound effects may improve by increasing the dose of the long-acting agent administered in the morning or adding a smaller dose of short-acting medication at the end of the day, before rebound symptoms typically occur Tics – Given the frequency of associated tic disorders and ADHD, the erratic and spontaneous star or end of tics, new or worsening tics maybe coincidental rather than caused by the medications. A brief trial off of medication or at a lower dose may be tried. The trial is most informative if the tics persist when the medication is stopped.



